Case 001 – Teenager with Early Root Formation of their Wisdom Teeth
We see a lot of patients interested in having their wisdom teeth removed at South Austin Oral Surgery. The Wisdom Tooth Consult series will review some of the cases that we have seen and go in depth regarding how the wisdom teeth are evaluated and the decisions that are made regarding options and treatment for these teeth. Patients age and sex may be slightly modified to better protect their privacy.
Patient Examination
Our patient is 19 year old male that was recommended to have his wisdom teeth out by his general dentist. He occasionally has mild discomfort with them, although he says that it is not too significant. The patient has no significant medical issues.
On exam, none of the patient’s wisdom teeth have broken through the gum tissue. They have clicking of the TMJ, but no pain. The panorex xray shows that all four wisdom teeth are full bony impacted. A tooth is considered impacted if either gum tissue or bone is covering at least a portion of the tooth. A full bony wisdom tooth is completely covered in bone. When looking at the top wisdom teeth, the roots are mostly formed, but not completely formed yet. You can see the end of the root still looks like a blob as opposed to a well-defined end seen in the neighboring teeth. The bottom wisdom teeth still don’t have any root formation. However, just under these developing lower wisdom teeth, you can see a band which is where the inferior alveolar nerve travels. This nerve provides feeling and sensation to the lower half of the face.
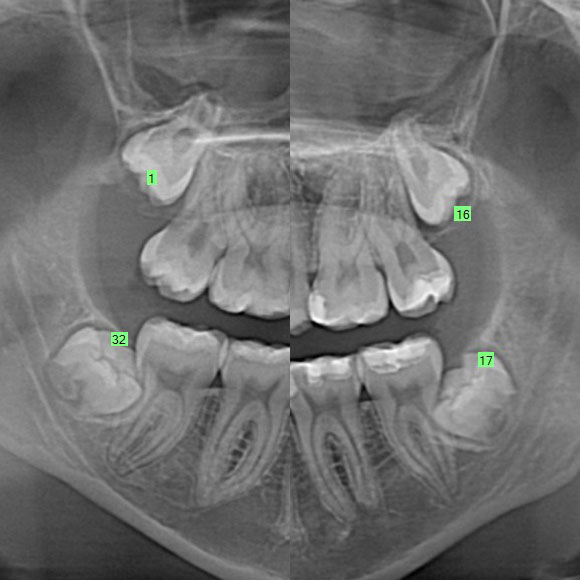
When deciding whether or not to treat wisdom teeth, we always need to look at the risks and benefits associated with removing them. Full bony wisdom teeth generally don’t cause issue as they are sealed off from the bacteria and debris in our mouth. They may cause occasional pain as teeth are erupting, but they are unlikely to become infected. However leaving impacted teeth can cause other issues in the future such as tooth resorption (a process where it eats away at the neighboring tooth) or pathology (cysts or tumors). These are unlikely to occur, but if wisdom teeth are left in place, they should be periodically evaluated with panorex xrays to make sure these processes are not happening.
Panorex X-ray Review and Evaluation of Findings
Upper Wisdom Teeth
For both upper wisdom teeth (#1,16), the roots have developed but the roots tips are still developing (red dots) and the crowns are not directed towards the teeth in front of them (purple arrow). They also don’t have enlarged follicles (yellow dots). Both of these indicate a lower risk for future root resorption or pathology. It is hard to predict if these teeth will stay impacted or potentially drift downwards and erupt into the patients mouth in the future. Having these teeth removed in the patient’s teenage years decreases the risk of future issues with them and also will result in better bone formation in the area where the wisdom teeth were. If these teeth require removal at a later age, the roots become more developed and occasionally develop hooks that makes removal more difficult and the bone around the wisdom teeth becomes denser. Removal at a later age also can result in poor bone regeneration in the space left by the tooth extraction which may ultimately affect the health of the tooth in front of it. There is no strong recommendation to either remove or leave the tooth in place for the upper wisdom teeth.
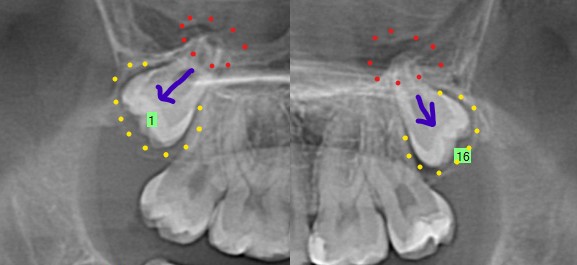
Lower Wisdom Teeth
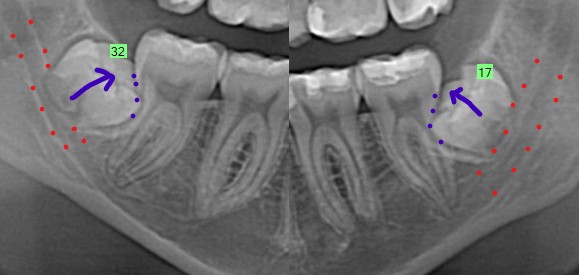
The lower wisdom teeth (#17,32) are still in early stages of development. Wisdom teeth are generally recommended for removal in teenagers when the roots are 50-75% developed – these wisdom teeth are at about 0% root development. However further root development in this patient will lead to an increased risk of nerve injury (nerve outlined with red dots) if the teeth need to be removed in the future. In addition, the teeth are slightly angled towards the teeth in front, so they have a higher risk of damage to these neighboring teeth through root resorption (purple dots). Due to the increased risk of nerve injury with further root development, this patient was strongly recommended to have both lower wisdom teeth removed. Sometimes, we recommend getting a dental CT scan to evaluate the relationship of the wisdom tooth and the nerve in 3 dimensions. However, I did not require this patient to get as it was not going change the treatment recommended or provided to the patient. Lower wisdom teeth removal can also put pressure in the TMJ. However since the roots are not developed and bone in younger patients tends to be softer, removal will result in less pressure placed on the joints during tooth removal.
Treatment
Our patient ultimately decided to have both the upper and lower wisdom teeth removed with IV sedation and placement of platelet rich fibrin (PRF) in both the lower wisdom tooth sites. The procedure itself went smoothly. The nerve was seen in the socket of both lower wisdom teeth, but was intact and not disturbed during the procedure. As a precaution, the patient was given steroids through his IV to further decrease the risk of nerve injury. We contacted the patient the following day and he confirmed that his facial sensation returned. No additional steroid treatment was required. The remainder of the patients recovery was without issues.
Dental Codes Used for Billing
Diagnostics
D0140 – Limited Exam
Surgery and Sedation
D7240 x4 (#1,16,17,32) – Extraction of Full Bony Impacted Teeth
D9222 – IV Deep Sedation, first 15 minutes
D9223 x3 – IV Deep Sedation, each additional 15 minutes
If you are looking for excellent care for your wisdom tooth removal in Austin, Texas, give South Austin Oral Surgery a call at (512) 692-7140.
Want to check out more cases in the Wisdom Tooth Consult series – click here !
